Do you sometimes have the feeling that your HbA1c results don’t really fit your expectations? Too high, too low? In this article, we’ll share some background information about how the HbA1c does not always tell the whole story.
The HbA1c can be elusive and determining the HbA1c value is sometimes like opening a mystery package. You can shake and shake as much as you want, but often the result is something completely different than you expected. So it is no surprise to learn that the HbA1c doesn’t tell the truth about blood sugar management?

The HbA1c often only tells half of the story
The HbA1c is often viewed as the number of numbers, the so-called gold standard. In general, it gives you and your doctor a rough impression of your blood sugar management over the previous 8-12 weeks. However, the HbA1c often only tells half the story, which is why it is worth taking a closer look behind the scenes of this often feared number.
Remember those early math skills you swore you’d never use? Time to brush up on those basics and review Averaging. First, you add all the values together and then you divide them by the number of values to find the average. That’s how an HbA1c is determined!
The HbA1c test is the measure of hemoglobin (red blood pigment) that is chemically bound to sugar. In people without diabetes, this value averages 5%. That means approximately 5% of the hemoglobin is saccharified (bound to sugar). The bonded amount of hemoglobin depends on the level of the mean blood sugar, i.e. an average! And since the HbA1c is really just an average, it makes sense that it consists of both good blood sugar values and numbers outside of the target range. In other words, a person with relatively stable blood sugars can have exactly the same HbA1c as someone in whom the blood sugar fluctuates to both extremes.
An HbA1c of 7.2% achieved with stable blood sugar values is not necessarily worse than an HbA1c of 6.7% achieved with large fluctuations. For our visual learners, we have illustrated this point in a graph:
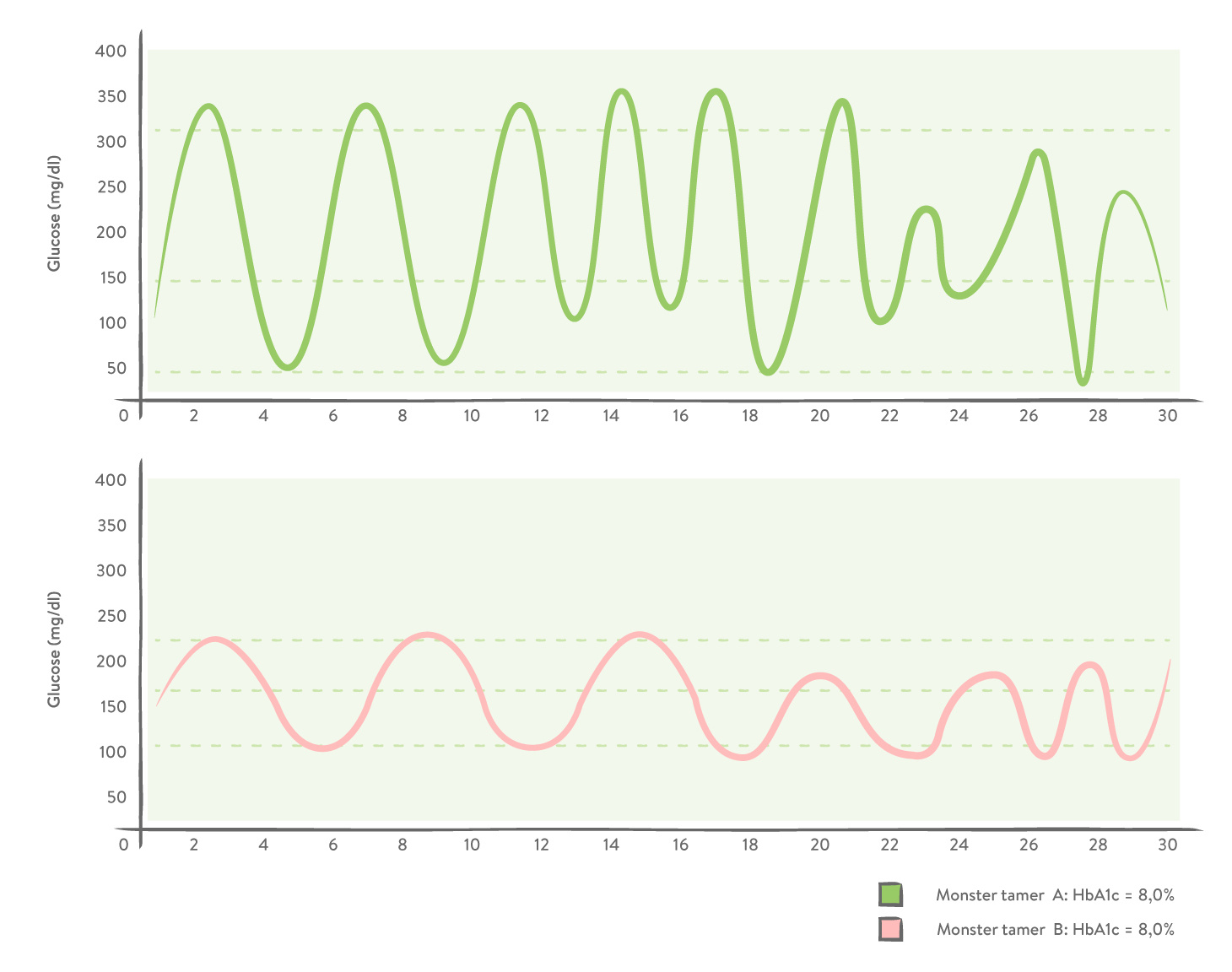
What happens between glucose readings?
Many people with diabetes only measure their blood sugar prior to eating. This allows those postprandial peaks (i.e. the blood sugar spikes after eating) to remain undetected. Therein lies the rub. These postprandial spikes in blood sugar, even if they are short in duration, can have a negative long-term effect on HbA1c.
Technology can bridge the gap!
Even if you believe that your blood sugar levels are always in range between your usual blood sugar checks, it is definitely worth doing a few extra checks from time to time. Ideally 2 hours post-meal for starters, and a morning fasting and bedtime check would be a wise addition as well.
For those of you utilizing CGM (Continuous Glucose Monitoring) or FGM (Flash Glucose Monitoring) in their arsenal, you can count yourselves lucky! CGM and FGM systems give you the opportunity to assess your metabolic situation in almost real-time. The trend arrows show you where your sugar is currently moving, which in turn enables targeted intervention. This allows for a tighter control and more Time in Range.
What influences HbA1c BESIDES glucose?
Believe it or not, there are some factors that can produce a false high or false low HbA1c values. As mentioned above, the HbA1c reading depends on the survival of the (sugared) red blood cells. The normal lifespan is approximately 8-12 weeks but it can vary from person to person due to hereditary “abnormal hemoglobin” or glucose-independent factors.
Causes of False High’s
If red blood cells live longer than expected the sugar has more time to combine with the hemoglobin in the red blood cells. This will cause a false high on your HbA1c test. A few non-diabetes-related reasons could be:
- Anemia from iron deficiency: A condition whereby insufficient red blood cells are formed. The few available will live longer and have more time to combine with the sugar.
- Impaired kidney function: Anemia also occurs here due to the reduced hormone production of the diseased kidney. Warning: HbA1c can increase up to 3% even in non-diabetics.
- Medications: Some medications can suppress the formation of healthy red blood cells. Immunosuppressants and Protease inhibitors can directly extend the lifespan of red blood cells. Likewise, high doses of ASA or certain antibiotics will also lead to false high HbA1c values.
Causes of False Low’s
Just as certain conditions or circumstances can cause false high’s, you can also have non-glucose-related low’s to your HbA1c Value as well. A few non-diabetes-related reasons could be:
- Acute blood loss: Whether it’s from benevolent blood donation, or due to an accident or operation, acute blood loss causes new red blood cells to form which have less time to bind to the sugar (saccharify).Fun fact; even a single blood loss of just under half a liter lowers the HbA1c by 0.5 for as much as 6-8 weeks.
- Dialysis (blood wash): Dialysis is a clinical purification of the blood. During this process the sugars has less opportunity to bind to the red blood pigment.
- Hemolysis and hemolytic anemia: A condition where the red blood cells are destroyed prematurely.
- Vitamins C and E: Long-term intake of vitamins C & E can inhibit saccharification of the red blood cells.
- High Altitudes
How mySugr can help to estimate your HbA1c
Here at mySugr, we know all too well that life with diabetes can be complicated. Almost ⅓ of our team lives with type 1 diabetes. We know that steering the HbA1c in the right direction is often a challenge.
This is why we strive to give you as much help as possible, to make diabetes suck less via the HbA1c estimate in the mySugr app. It can differ from a laboratory value, but the more blood sugar values you enter in the mySugr app, the more accurately we can estimate your HbA1c value in between your regular doctor visits.
Small improvement - big impact
As in everything else with diabetes therapy, knowledge is power. Even small improvements in therapy, such as avoiding postprandial peaks, can have a major impact. The HbA1c by itself may not say enough about the actual blood sugar management, but it’s a start. You can dig a little deeper by evaluating the time in the target area (Time in Range / TIR) and the standard deviations within your own body. Add in the right tools and the support of your medical team and you’ll be well on your way to better health!
Monster tip: The nightly sleep phase makes up a large part of your overall blood sugar setting. ⅓ to be exact. So if you manage to keep your blood sugar levels stable at night, you will already have ⅓ of your HbA1c value in the bag.
The mySugr website does not provide medical or legal advice. mySugr blog articles are not scientific articles, but intended for informational purposes only.
Medical or nutritional information on the mySugr website is not intended to replace professional medical advice, diagnosis or treatment. Always consult a physician or health care provider with any questions you may have regarding a medical condition.





